|
INCONTINENCE & THE PROSTATE
(from Morganstern Urology Clinic & Men's Health Center)
Types of Prostate-Related Incontinence
Problems of Incontinent Men
The Extent of Incontinence
How Prostate Treatment Can Cause Incontinence
Managing Incontinence After Prostate Treatment
Absorbent Products
Artificial Sphincters
Catheters
Drugs
Kegel Exercises
External Collection Devices
Injections (e.g., collagen)
Reconstructive Surgery
Types of Prostate-Related Incontinence
Broadly defined, incontinence is the loss of voluntary control over
passing waste products from the bladder and less commonly from the bowel.
Here, we'll deal only with urinary incontinence, the inability to consciously
control urine flow from the bladder.
Incontinence associated with prostate treatment may be either temporary
or permanent. Temporary incontinence and occasional passage of blood in
the urine happen to almost all patients after they have prostate surgery.
As they heal, incontinence and bleeding often go away, sometimes while
they're still in the hospital or within a few weeks after they get home.
Unless your urologist observes strong indications to the contrary, never
conclude you are permanently incontinent unless your condition persists
and shows no signs of diminishing for at least six months after transurethral
resection, radical prostatectomy, or radiation treatment. With modern techniques,your chances of permanent incontinence are no more than 1.5 percent in the case of a TURP, and 2 percent with radical prostatectomy. Following
radiation therapy, your chances of incontinence are typically less than
5 percent.
Incontinence can have several different forms. But following prostate
surgery, it is usually of the "urgency" type, occurring when
there is a sudden, uninhibited contraction of the bladder. Urgency incontinence
gives you virtually no warning of the impending expulsion of urine, so
you have no time to reach the bathroom.
More than half of all incontinence cases in both men and women are believed
to be "stress" incontinence, a condition somewhat less serious
than urgency, and characterized by the insignificant loss of urine following
laughter, coughing, lifting heavy objects, or straining the body physically
in other ways. Men may experience some degree of stress incontinence after
prostate treatment, but not as severe as urgency incontinence.
Some men may experience a condition known as "overflow" incontinence,
sometimes known as "paradoxical" incontinence, characterized
by the frequent, temporary inability to void when the need is apparent,
followed by uncontrollable urine flow. Typically, the flow is at a slower
rate than is the case with urgency incontinence. Overflow incontinence
is a condition that can be caused by prostate enlargement and is not a
consequence of surgical or radiation prostate treatment. If you experience
symptoms of overflow incontinence, you should consult a urologist.
Two other conditions are "functional" and "iatrogenic"
incontinence. The former occurs when men are unable to make it to the bathroom
on time owing to physical injury or psychological problems, a condition
common among older men confined in nursing homes. The iatrogenic form is
associated with drugs, including certain antihistamines, heart disease
and blood pressure medications, tranquilizers, and muscle relaxants. Men
who have had surgical or radiation prostate treatment, may experience either
functional or iatrogenic incontinence, but not usually because of prostate
treatment.
Problems of Incontinent Men
Problems associated with incontinence include inconvenience, discomfort,
and hygienic consequences, all manageable and sometimes curable, so normally
there should be no physical reason keeping you from living a full and active
life if you should become incontinent after prostate treatment. Unfortunately,
many men have hard time coping with the emotional consequences of incontinence.
Homer, a 50-year-old commercial photographer, became permanently incontinent
after transurethral resection. He had been a good patient, but when the
permanence of his condition became apparent, he became increasingly depressed,
did his best to avoid all social contact, and began to drink heavily.
Discussing his problem with Homer, I learned he had been raised in a
very authoritarian home where bedwetting was a point of great contention.
His parents had tried to toilet train Homer well before the age of two
and he still remembered being shamed by his parents after frequent accidents.
In treating him, I had to address both Homer's emotional and his physical
difficulties. He benefited almost at once when I told him his childhood
bedwetting was not his fault, nor was it a disgrace. Surgical implantation
of an artificial urinary sphincter resulted in effective physical control
of Homer's incontinence. In a few months, Homer's emotional state had improved
greatly and he was enjoying a fully acceptable life-style.
Homer is not unusual. Despite a trend toward more enlightened attitudes,
society still places a premium on early toilet training and regards a child's
incontinence as a failing. Consider the popular conservative radio talk
show host who uses the term "bedwetter" as a pejorative, someone
akin to a wimp, or maybe a liberal.
If you do experience prostate-related incontinence, it will definitely
help you if you are familiar with the connection between any early and
aggressive toilet training and your emotional reaction as an incontinent
adult. Everybody is incontinent at birth, but by age three, most children
are well on their way to bladder control, with only minimal effort by their
parents. In fact, most physicians will not conclude a childhood incontinence
problem actually exists until loss of bladder control occurs daily well
past three. However; occasional mishaps are normal to all young children.
Pushing toilet training too early and making too much fuss over an occasional
mishap may instill a feeling of guilt and shame in a young child that can
last a lifetime.
It may also help to put in proper perspective the issues of spreading
disease and giving offense. Contrary to popular belief, urine is normally
sterile and, absent of any infectious microorganisms, will not spread
disease. Also, urine will not smell unless there is infection or some other
abnormality. But urine can be dark yellow, which may make more apparent
accidental staining of your underwear and trousers. Dark-colored urine
usually results from drinking insufficient water. Dark urine sometimes
scares incontinent men into drastically limiting their water intake in
the mistaken belief that it will help alleviate their condition.
The Extent of Incontinence
Some estimates suggest as many as eleven million American men and women
may have an incontinence problem. Women may account for more than half
the total cases. The precise dimensions of this problem are not known.
However, it is likely that fewer than half of all incontinent individuals
ever seek medical treatment, which adds considerable uncertainty to estimates.
Of course, many individuals have only borderline symptoms and do not bother
to seek help, and when they do, there is a question whether their symptoms
should be classed as permanent incontinence.
Among American men, prostate treatment is an important element in permanent
incontinence. There are no hard figures, but some estimates suggest as
many as 1.5 to 2 million American men may have a permanent incontinence
problem possibly related to prostate surgery or radiation therapy. On that
basis, prostate surgery could be a factor in about a fourth of all incontinence
cases in adult males. As discussed below, there may also be multiple causes.
Treating adult incontinence in the United States has become a growth
industry. If you doubt that, just watch primetime televison some evening
and see if there aren't several commercials for adult incontinence products.
The number of incontinent individuals is growing, owing to the continuing
upward trend in the average age of Americans. The relative importance of
prostate treatment in the overall incontinence picture will probably decline
though, as improved surgical and radiation techniques continue to be developed.
How Prostate Treatment Can Cause Incontinence
To see how prostate surgery may result in incontinence, let's take a
quick look at human urinary plumbing. In men and women both, the urinary
process begins in the kidneys, a pair of vital organs whose main function
is to purify your blood. Blood flows continuously into each of your two
kidneys through the large artery known as the aorta. Once inside the kidneys,
blood is filtered and any impurities are removed. The purified blood is
recirculated into the bloodstream. Roughly 10 percent of the fluid volume
of blood entering the kidneys becomes urine that carries these filtered
impurities outside your body. Urine exits from each kidney and flows to
the bladder through two ducts called ureters.
In effect, the bladder is a storage tank that holds a continuously increasing
volume of urine until a buildup of pressure sends a signal to your brain
indicating the need to void. At the base of the bladder is the urethra,
the pipeline that carries urine outside your body. In men, this outlet
passes first through the prostate and then through the penis. In both men
and women, two circular muscles known as sphincters serve as valves that
control urine flow from the bladder. If all is well, the valves close normally
and urine is retained until voiding is socially convenient. When you are
ready to void, your brain sends a message through the somatic or conscious
nerve circuits ordering the valves to open and then you can urinate.
The average adult male passes about one quart of urine a day. Over an
average lifetime, that adds up to somewhat more liquid than would fill
a standard, above-ground, 18-foot-diameter swimming pool. Given the amount
of work performed constantly by your urinary system it is hardly surprising
that some form of trouble, like incontinence may eventually occur.
In men, incontinence can be caused by a number of factors: prostate
enlargement, diabetes, spinal-cord injuries, spina bifida, strokes, multiple
sclerosis, certain drugs, and other conditions that impair the critical
sections of the nervous system controlling voiding. Proper function of
the urinary sphincter muscles is sometimes impaired by physical injury,
urinary infections, or by an obstruction at the bladder outlet. Muscle
function may also decline over the years from the natural aging process.
In some incontinent individuals, psychological factors may also be present.
When incontinence follows prostate treatment, the usual cause is surgical
damage to the urinary sphincter muscles, impairment of the nerves controlling
sphincter action, or some combination of both. The anatomy around the prostate
is very crowded so that, even with the most advanced surgical techniques,
avoiding some damage to nearby healthy tissues during a transurethral or
radical prostatectomy is almost unavoidable.
When prostate treatment causes serious damage to the sphincter, it usually
remains fully or partially open. A constant dripping form of incontinence
is a typical result. As might be expected, the leak tends to be especially
bad when standing or sitting, tapering somewhat when you lie down.
Most men who require major prostate surgery are usually of an age when
there is a strong possibility of incontinence from causes other than surgery.
In my practice, I always investigate the bigger picture because some factor
other than surgical damage may contribute to the problem. The condition
may be caused or complicated by a so-called irritable bladder, a neurological
problem. Under those circumstances, treating that additional factor may
result in a marked improvement in the patient's condition. Simple tests
can diagnose many of the additional factors that may contribute to incontinence.
Managing Incontinence After Prostate Treatment
With the many methods now available to manage incontinence, effective
solutions are possible for every patient.
Absorbent Products
Absorbent products are the most common way to deal with incontinence.
They are easy to use, readily available, and fairly inexpensive.
A number of absorbent products on the market are designed to be worn
under normal street clothing. For men with a minor incontinence problem,
a drip collector (a pouchlike device worn over the penis) may be sufficient.
Shields, a product resembling a feminine menstrual pad, are designed for
individuals with light to moderate loss of bladder control. Adult undergarments
are products like diapers and are intended for individuals with moderate
to severe control loss. For those with either minimal or complete loss
a fitted garment known as a brief, resembling regular underpants, is also
available.
All these products have their pluses and minuses, including varying
degrees of comfort and protection, ease of disposability, and how convenient
it may be to carry an adequate supply while engaging in normal activities.
Recently there has been fierce competition between two well-known companies,
Kimberly-Clark and Procter & Gamble, to dominate the growing, adult
incontinence market. Although their television commercials can be annoying,
there is little doubt that this competition has brought about development
of less bulky products offering improved absorbency, better comfort, and
other desirable features.
Artificial Sphincters
Artificial urinary sphincters are a bagel-shaped prostheses designed
to be surgically implanted in incontinent men or women. Once in place,
this device surrounds the urethra in the same general area as the natural
sphincter. A quantity of hydraulic fluid in the prosthesis applies continuous
inward pressure on the urethra, choking off urine flow from the bladder.
In incontinent men, a small bulb is hidden within the scrotum. The fluid
in the prosthesis is connected to the bulb through a narrow tube. When
a man has an urge to urinate, he merely squeezes his scrotum in the vicinity
of the bulb, which releases pressure inside the artificial sphincter and
permits urine to flow from the bladder. A few minutes after voiding, fluid
pressure within the prosthesis returns automatically to its normal level,
once again preventing urine flow.
When performed by a competent urologist, artificial sphincter implantation
is relatively simple and usually successful. When performed in a hospital,
the procedure involves only a two- or three-day stay. Under appropriate
anesthesia, the operation is painless and involves minimal surgical risk.
A very small number of patients may experience some minor post-operative
discomfort and possibly some treatable local infection. Depending on your
location, the medical facility you select, and related factors, the procedure
can cost less than $10,000, and should be covered by most insurance policies.
Artificial sphincters are made from the same inert, silicone plastic
materials and are usually manufactured by the same companies as the penile
implants in Chapter 7. Safety concerns about female silicone breast implants
have not been raised with either artificial sphincters or penile implants
because silicone-containing fluids in breast implants are not used with
either of these devices.
An artificial sphincter implantation is highly suitable for a broad
spectrum of patients. I have men patients in whom I have successfully installed
both artificial urinary sphincters and penile implants. Adequate room exists
within the body for both devices and even then, there is little visual
evidence of their presence nor do they represent a major obstacle to normal
physical activities.
Catheters
In effect, a urinary catheter is a tube that for men is inserted
through the tip of the penis into the urethra. The best known is the Foley,
a device often employed with hospital patients recovering from surgery.
The tip of the Foley is inserted until it enters the bladder. A small bulb
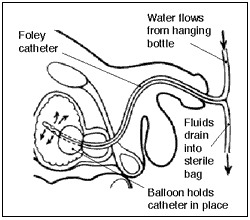 at the tip, when inflated, holds the tube in place. Once it's secure, urine
flows continuously into a concealed leg bag or some other container.
at the tip, when inflated, holds the tube in place. Once it's secure, urine
flows continuously into a concealed leg bag or some other container.
However, extended use of a Foley catheter can cause unpleasant irritation
at the tip of the penis. The device can also cause urinary tract infections
and bladder stones, so it is generally recommended only under continuing
medical supervision. Most interest nowadays centers around intermittent
catheters, which are inserted only from time to time. Typically, these
devices are removed and reinserted every four hours or so.
Intermittent catheters are especially common in patients with spinal
cord injuries. For post-surgery prostate patients, intermittent catheter
use is well accepted. Many men are easily capable on their own of learning
to manage this removal and reinsertion process. In men where age, physical
condition, or sensitivity is a problem, these devices are generally inappropriate.
Drugs
Drugs for treating incontinence are in their infancy. Those investigated
are meant to cause either increased constriction at the bladder outlet
into the urethra or to prevent excess contractions higher up in the bladder.
Antihistamines, for example, can improve muscle tone at the neck of the
bladder; which is why men with incontinence sometimes notice an improvement
when they take over-the-counter antihistamines for the relief of common
colds or allergies.
Other drugs that have been tested include the antidepressant impramine
and propantheline bromide for treating peptic ulcers, sold under the name
Pro-Banthine. Unfortunately, many of the drugs investigated so far have
undesirable side effects. Antihistamines frequently cause dizziness and
a degree of sedation, so they should be used cautiously in patients with
asthma, cardiovascular problems, and other conditions. Impramine can cause
cardiac problems, weakness and fatigue, allergic reactions, and other symptoms.
Propantheline bromide is associated with cardiac problems and should also
be avoided by glaucoma patients.
Generally, drugs for treating incontinence are not too effective when
damage to the sphincter muscles from prostate surgery is severe. They may
help where the damage is relatively minor or where other factors contribute
to incontinence. But the pace of research in this area is accelerating
and it is likely that more effective and safer drugs will eventually become
available.
Kegel Exercises
Kegel or pubococcygeal exercises, dating to about 1950, were developed
originally by Dr. Arnold H. Kegel, a gynecologist, who expected they would
help women overcome episodes of incontinence after childbirth. Later the
same exercises were found to help incontinent men, too, including those
who had prostate surgery. br>
Kegel exercises are performed by tensing and tightening the pubococcygeus
muscle in the vicinity of the rectum. Even if its name is unfamiliar, you
have been aware of it most of your life - this is the muscle you feel whenever
you strain to start or stop your urine flow while voiding. You can learn
to do the Kegel properly by using the muscle repeatedly to interrupt your
urine flow. In time, you will no longer need to urinate by exercising the
muscle and can even make your penis bob up and down without using your
hands.
Quick Kegels consist of rapidly tightening and relaxing the muscle.
In slow Kegels, the muscle is tightened to a count of five, then relaxed.
Four sets of each exercise should be performed each day, with the number
of Kegels per set gradually increased. For all you know, you may once have
talked to someone who was quietly doing some Kegels, because the exercise
can be performed without attracting attention whether standing or sitting.
Positive results may take up to three months, but after that a Kegel or
two immediately before getting up from a chair or hearing a great joke
may help avert an accident.
There have been some claims that the Kegel also provides sexual performance
benefits. Some women who practice the Kegel are said to enjoy greater pleasure
during intercourse, along with their partners. Men who practice the Kegel
are said to have better ejaculatory control. It is difficult to substantiate
these claims, but there is no reason not to try them yourself.
Kegel exercise devices made of rubber-coated steel are also available
for about $35. The device is designed to be held tightly in the crotch.
By squeezing the device, more tension is presumably placed on the muscle
than during a normal Kegel. However, most authorities don't believe the
device is worth its cost.
External Collection Devices
Incontinent men have one obvious advantage over women when
it comes to external collection devices. A typical device for men is made
of soft rubber and resembles a condom, which is pulled over the penis and
held in place by a band around the waist. A drainage tube connects the
device to a collection bag secured to one of the user's legs by a band.
An external collection device can also be used with a penile clamp to control
urine flow.
External collection devices are a relatively inexpensive means for dealing
with incontinence. However, many men find them uncomfortable and cumbersome.
For some, there may also be a problem in achieving adequate physical connection
between the penis and the device. I have corrected that problem in several
cases with a semirigid penile implant (see Chapter 7). With the implant
in place, there is adequate extension of the penis to produce a tight connection
and the implant also provides a workable solution for simultaneous impotence
problems.
To avoid infection, external collection users are cautioned to clean
themselves frequently and to replace parts of the system regularly. Men
who use a penile clamp with an external collection device are cautioned
not to apply too much pressure because they might dangerously restrict
blood flow through the penis. Some men swear by external collection devices,
while others, for the reasons indicated above, swear at them.
Injections
Collagen is a naturally occurring protein found in the connective
tissues that make up the joints and the bones of animals, including humans.
Common gelatine desserts are mainly flavored collagen.
Some incontinent men are helped when small quantities of highly purified
collagen are injected into the neck of their bladders. Polytef, a synthetic
substance based on silicone, has physical properties similar to collagen,
and is sometimes used in this manner.
Typically, a series of several injections is required before any improvement
is noted. The procedure is simple, causes minimum discomfort, and is relatively
inexpensive.
Reconstructive Surgery
Unfortunately, until recently, the results from reconstructive surgery
to correct incontinence in men whose sphincter muscles were damaged by
transurethral or radical prostatectomy have generally been discouraging.
Research is still underway in this area and it is likely that with improvement
in surgical techniques, an increasing number of men should be helped by
this surgery.
At this stage, reconstructive surgery is limited to experimental procedures
designed to strengthen and reinforce the sphincter muscles. No techniques
yet exist to repair damage to the sphincter nerves. Ask your urologist
whether reconstructive surgery offers any real promise in your case. If
so, you will probably be referred to a specialist.
|
|